Leveraging Narrative Strategy for Health and Racial Equity: The NYC Bureau of Chronic Disease Prevention’s Journey
A conversation between Human Impact Partners and New York City Health Department’s Bureau of Chronic Disease Prevention

At Human Impact Partners, we believe that the language we use to talk about health and wellness matters. Dominant public narratives about what health means and where it comes from affect programs and policies and shape what sort of futures we imagine are possible. Part of our work as public health practitioners is dismantling narratives that prevent us from achieving health and racial equity and creating new transformative narratives to guide our vision of a just world where all people can flourish.
In this blog post, we’re highlighting the narrative work of the New York City Department of Health and Mental Hygiene’s Bureau of Chronic Disease Prevention (BCDP) as an example of how public health departments can successfully incorporate narrative change into their work to achieve health and racial equity. For the past half decade, the Bureau has embarked on a journey to reimagine how it tells the stories of what creates health and think critically about its data presentation and analysis. The murder of George Floyd and the widespread devastation and stark inequities caused by COVID compelled the Bureau to dive even more deeply into this work. Throughout the process, which has involved and engaged all staff, the Bureau has evolved from its initial focus on health disparities to incorporate a broader critical analysis of the structural and systemic roots of health inequity into its work.
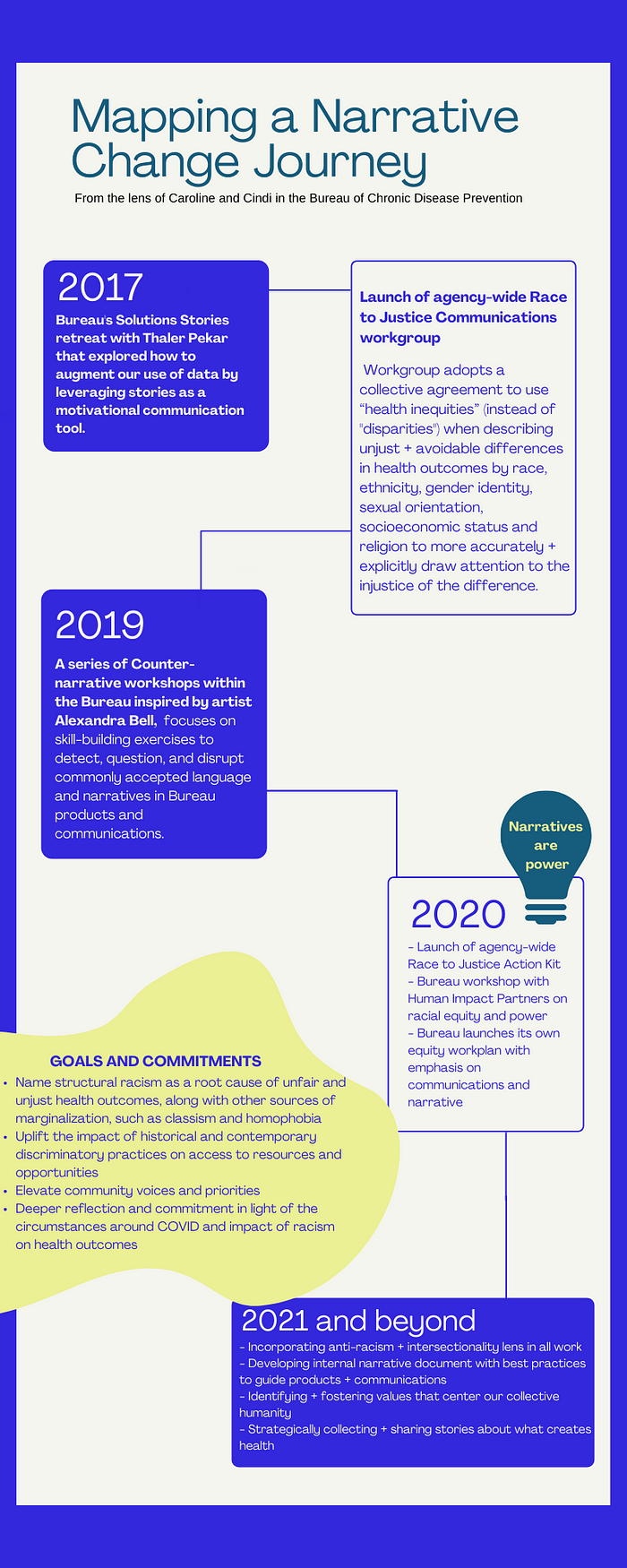
We sat down with Cindi Azuogu and Caroline Miller — both with the Bureau of Chronic Disease Prevention — who have been champions of narrative change efforts and worked closely with Human Impact Partners to integrate new practices across the Bureau’s work. We talked in depth about what they’ve learned from their narrative journey, the challenges they’ve faced, and how other public health agencies can incorporate narrative work into their practice.

The following conversation, edited for length and clarity, captures the personal reflections of Cindi and Caroline. The interview was conducted by Lili Farhang and Clara Liang of Human Impact Partners.
Is there one moment or event throughout your narrative work journey that made you realize how important narrative work is to health equity?
Cindi: My pivotal moment was during the protests and uprisings around the murder of George Floyd in 2020. Not only was his death very public — the activism around his death was, too. It felt really disorienting, the way everyone tuned in to watch the spectacle of Black death on which this country is founded.
This moment really challenged me to realize that in some ways our public health work perpetuates this spectacle. I began asking myself, how is public health talking about Black people and their experience of this kind of race-based violence? Maybe we’re not displaying it on television or YouTube or social media, but in what ways are we further undignifying Black people through how we talk about Black bodies, Black death, and Black health?
The way public health talks about Black death — “Black people are more likely to die of this, this, this, and this” — began to feel like a real failure to communities that already experience far worse health outcomes.
Often, health disparity research is what gets funded because it supports that narrative of sick people being Black people, Latino people, people of color, people who are low income. That’s what gets you grants. But reinforcing this narrative becomes a perpetuation of the systemic problems that we are trying to solve. I think by shifting the narrative, we can shift our projects and funding to actually create change.
Caroline: A pivotal moment for me was in 2019, when the Bureau did a series of workshops that we called Counternarratives. They were inspired by artist and journalist Alexandra Bell, who did a series of the same name where she analyzed New York Times headlines looking at how people were being represented based on their race, ethnicity, and heritage.
We adapted this exercise and used it to reflect inward. We examined our own materials by deconstructing language used in data reports, press releases, presentations and health resources. We interrogated our use of disparities data and how we present it to different audiences.
It was an empowering experience. This exercise enabled some of our staff to see their own roles in shaping the narratives that we put out into the world. It made us realize that we could reflect with greater intentionality on how and what we communicate and purposely shift, as individuals and as a government agency, the narrative around what creates health.
What has been the most gratifying part of your narrative change work?
Caroline: In my experience, this narrative work transcends the traditional hierarchy that is characteristic of government in general. This work has offered entry points for many different people in our Bureau and across the agency to join and offer valued expertise and experiences, regardless of level of seniority. Each person truly comes in as an expert, reflecting on their own experiences and identities. The work has modeled a new way of collaborating and generating deliverables within our Bureau. It’s served as a unifying thread for us, as a team that covers so many chronic disease prevention topics and uses different approaches and interventions. It’s a body of work that doesn’t sit with just a few people. I’ve seen a growth in a sense of collective ownership of the narrative work.
What has been the most challenging part of this narrative work?
Cindi: One instance that comes to mind is when we were trying to create a narrative about hypertension prevention and control to include in presentations to community-based organizations. Initially, we wanted to exclude the early death data from New York City about how Black people die at higher rates and have higher rates of strokes and heart disease because it felt undignifying. But when we met with our hypertension team, a colleague stressed that this is real information the community deserves to have, and that it’s the Department of Health’s responsibility to not only collect this data but to share it so that communities are aware of what’s happening. Because this is a tragedy. It’s a loss. It’s not something that we can just delete from a presentation and pretend it doesn’t exist. We just need to be aware and transparent about our commitment to doing something about it.
Hearing that conversation about how important it is to be accountable to communities, to share the information that we collect so they know they’re being seen, that was a big moment for me.
We started to shift our framing of hypertension prevalence and mortality data to focus less on simply presenting the numbers and sharp contrasts by race/ethnicity to elevating the sentiment, “We see you, this is not ok, and we’re committed to figuring out how to change these numbers.” Two narratives, same data. That was such an eye-opening moment for me.
So the challenge is, how do we make people feel seen and center their humanity in our work?
Can you talk about how your narrative strategy work has changed how you think about, assess, and share public health data?
Cindi: Now, our team is being way more thoughtful about how we share data and what the numbers say — ultimately, data represents people and we want the data to reflect their humanity.
We’re creating a guide for our documents, publications, papers — all the things that carry narrative — with practices to consider, like, “If you show the disparities exist, make sure to explain why they exist.” This work has helped me be very purposeful about what story we’re trying to tell — this is the stance we’re taking, this is what we believe in, rather than “You are more likely to die of x, y, z, now let’s move onto the next data point.”’
You’ve talked about how the process of doing this work has been as important as the outcomes. Tell me more about that.
Caroline: I think the narrative work has forced us to constantly interrogate our “go-to” practices and bring more intentionality to all our decision points. It’s allowed us to be in a place of constant learning and evolution.
A few years ago, there was a clear directive across the agency to name racism more in our work. But the way that that often got translated was naming disparities by race and ethnicity without offering the context and naming the inequities. From there, we pushed ourselves to not just name disparities but also the structural forces — whether that’s racism or another system of oppression or power imbalances — at the root of health inequities. And then we learned that the presentation of data, even with structural framing, can still be demoralizing and dehumanizing. So we pushed ourselves even further to ask, how can we center peoples’ humanity in our data presentations and how we talk about health inequities?
Human Impact Partners has been an invaluable partner in pushing our internal thinking throughout the process. We continue to build on the work, each step of the way, whether it be through application of the Agency’s Race to Justice Action Kit, or through creation of best practices for our Bureau’s use to further shift our products and communication strategies systematically. Individual teams within our Bureau — hypertension, cancer, active design, tobacco, nutrition and others — are going through their own learning processes and engaging with these questions.
Cindi: Narrative work really feels like a transformative process. It’s extremely gratifying to feel like I’m being part of the solution. Because this work doesn’t require a master’s degree — it really just requires reflection on yourself and the world around you and how you fit in. I love the idea that anyone can be part of the solution. It helps me feel grounded. It’s an empowering feeling.
Working in a Department of Health, I forget I’m also a citizen, and that in some way, what we put into the world will also impact us as public health workers. So slowing down and incorporating the language of love into our process has been a reminder that we are inextricably linked in everything we do — that we’re not free until everybody’s free, we are all bound to each other’s freedom. That’s such an important reminder when doing this work.
What are the Bureau’s next steps in this work?
Caroline: While it’s been ongoing for years, it feels like we’ve only just begun! We’ve done the initial leg work of disrupting common practices and identifying opportunities for change, and now we really need to test things out and have the confidence and will to be bold about it.
We’re continuing our work with HIP to receive technical assistance on communication practices and to reflect as a Bureau on our values as an organization, so that when we shift narrative we have a set of grounding ideas and commitments to guide us.
Cindi: I’d add that developing narratives is just one part of this journey. Embodying the narratives is another. We can say that we are an anti-racist institution or organization, we can declare racism is a public health crisis — but if the workforce that makes up the organization is still treated in inequitable ways, the narrative we have created starts to lose meaning. My passion for public health is in the praxis — how are we living out and practicing the principles of health equity? I’m looking forward to doing the work of ensuring the theories of health equity meet the practice.
What advice would you give to staff at other public health organizations who are working to develop a narrative of their own, and to shift dominant narratives about health?
Cindi: Start with yourself! See what comes up when you think about the narratives that come up in your own heart and mind, then think about the work and social environments you exist in. What narratives are developed in those spaces and how do they impact your worldview? What needs to be strengthened? How can we share our narratives out intentionally?
Caroline: Consider how the ways in which you are currently describing your work may be limiting the possible solutions to the public health challenges you’re trying to tackle. Narrative change work feels like an organizing tool. It’s not just the work of communications teams or data analysts, it’s a way to organize a collective workforce around a shared goal. Ultimately, I really believe that words matter — what we put to paper and say to the world, how we communicate about our work — those words directionally pave where we want to go. That’s an empowering way to catalyze action.
📌 Did you know? Human Impact Partners provides health equity capacity building to public health organizations. Contact us to learn more about our offerings at info[at]humanimpact.org.
